Understanding Senile Dermatitis: Challenges in Aging


Intro
Senile dermatitis represents a cluster of skin changes stemming from the aging process. As individuals age, their skin undergoes various transformations that may lead to distinct dermatological challenges. Understanding these changes is vital for developing effective management strategies to enhance skin health among the elderly.
This condition is not merely cosmetic; it can significantly affect an individual's quality of life. Skin alterations can lead to discomfort, inhibit mobility, and even contribute to psychological distress. Consequently, a thorough understanding of senile dermatitis is essential for healthcare professionals seeking to provide optimal care.
The exploration of senile dermatitis encompasses a multitude of aspects, including its underlying mechanisms, varied clinical manifestations, and current therapeutic approaches. By delving into these topics, the following sections will elucidate the nature of senile dermatitis and its implications, particularly for aging populations.
As we proceed, it is crucial to emphasize the importance of timely diagnosis and intervention. By implementing appropriate treatment modalities, we can mitigate the impact of senile dermatitis and enhance the overall well-being of our aging population.
Prelims to Senile Dermatitis
In recent years, there has been a growing focus on senile dermatitis, particularly as the global population ages. Recognizing the unique characteristics of this condition is essential for effective dermatological care. This section intends to provide a foundational understanding of senile dermatitis, laying the groundwork for exploring its implications, management, and relevance to aging individuals.
Defining Senile Dermatitis
Senile dermatitis refers to skin changes that occur as people age. It encompasses various dermatological phenomena that arise due to intrinsic and extrinsic factors. Intrinsic factors include alterations in skin structure, such as a decrease in collagen and elastin, while extrinsic factors involve environmental influences like UV exposure and pollution. The result is skin that may appear thin, dry, or inflamed. Understanding the definition and scope of senile dermatitis enables healthcare professionals to recognize and address its manifestations effectively.
Importance in the Aging Population
The significance of senile dermatitis in the aging population cannot be overstated. As individuals grow older, their skin undergoes multiple changes that can lead to various dermatological conditions. This influence is particularly pronounced among older adults, who often experience a decline in skin barrier function, making them more susceptible to irritative and allergic reactions. Furthermore, the emotional repercussions linked to visible skin changes, such as embarrassment or diminished self-esteem, can adversely affect mental health. Therefore, the management of senile dermatitis and its related outcomes is not solely a matter of cosmetic concern; it is crucial for enhancing the overall quality of life in older adults.
This section sets the stage for a deeper exploration into the details of senile dermatitis, its epidemiology, pathophysiology, clinical manifestations, and management strategies. Understanding these components is essential for medical professionals engaged in caring for aging populations.
Epidemiology of Senile Dermatitis
Understanding the epidemiology of senile dermatitis is crucial for effective management and prevention strategies. This field of study highlights the distribution and determinants of skin changes associated with aging. It provides insight into how widespread this condition is among various populations, thus revealing its significance in public health. Given the increasing aging population globally, this topic becomes even more relevant. Adequate knowledge of epidemiological trends informs healthcare providers and researchers, which can lead to better-targeted interventions.
Prevalence Among Different Age Groups
Senile dermatitis can manifest differently across various age groups. Studies show that skin changes begin to appear in middle age, but the prevalence increases significantly as people reach their 70s and older. It is essential to recognize the different stages that aging skin goes through. For instance:
- In individuals between 50 to 60 years, early signs may include dryness and slight thinning of the epidermis.
- By the time one reaches the age of 70, dermatitis often presents with more pronounced symptoms such as chronic dryness, flaking, and redness.
- In elderly individuals, particularly those above 80, the skin may show severe changes, including increased fragility and heightened susceptibility to infections.
The prevalence data suggests that nearly 60% of older adults may experience some form of senile dermatitis in their lifetime. This makes it imperative to prioritize research and healthcare resources towards this demographic.
Demographic Variations
Demographic variations of senile dermatitis illustrate how factors such as gender, race, and geographical location can impact the condition.
- Gender: Studies report that women are often more affected by senile dermatitis than men. This could be related to hormonal changes, particularly after menopause, which can exacerbate skin conditions.
- Race: Certain ethnic groups may experience different levels of skin pigmentation and resilience, affecting their susceptibility to skin disorders. For example, individuals of European descent might display more signs of photoaging versus those with darker skin tones.
- Geographical Location: An individual’s environment plays a pivotal role. Those living in sunny climates may require more rigorous sun protection measures, thus reducing the risk of senile dermatitis.
These variations highlight the necessity for healthcare providers to consider individual risk factors during assessments. It also underscores the importance of tailored prevention strategies to mitigate the impacts of senile dermatitis.
"Analyzing the epidemiology of senile dermatitis is vital for the development of effective clinical practices to address the unique challenges it presents across different demographics."
Understanding these elements not only fosters better patient care but also strengthens the foundation for future research in dermatological health.
Pathophysiology of Senile Dermatitis
Understanding the pathophysiology of senile dermatitis is crucial in grasping the overall impact this condition has on the aging population. A detailed examination of how skin changes occur with age allows us to identify suitable management strategies and preventive measures. With aging, the skin undergoes various transformations that predispose it to dermatitis. This section sheds light on the biological processes involved and their implications for dermatological care.
Skin Structure Changes with Age
As people age, the skin undergoes significant structural changes. The epidermis, which is the outermost layer of the skin, tends to become thinner. Additionally, the rate of cell turnover decreases. This slowing down of cellular regeneration leads to a more fragile skin barrier. Consequently, older skin is more susceptible to irritants and allergens, which can exacerbate the condition of senile dermatitis.
Moreover, the dermis, which lies beneath the epidermis, also deteriorates with age. It loses collagen and elastin, the proteins that provide skin with strength and elasticity. This loss weakens the skin’s support structure, leading to increased sagging and wrinkling. These structural changes are vital to understanding why older adults often experience a greater incidence of skin irritations and dermatitis.
Role of Collagen and Elastin Degradation


Collagen and elastin are essential for maintaining skin integrity. In senile dermatitis, the degradation of these proteins plays a pivotal role. Research indicates that with age, there is a notable decline in collagen synthesis. This process is largely influenced by both intrinsic aging and extrinsic factors such as sun exposure and pollution.
The reduction in collagen can impair the skin's ability to retain moisture, leading to dryness. When the skin becomes dry, it can easily crack, leading to a series of inflammatory responses that worsen dermatitis. Similarly, elastin degradation contributes to diminished skin resilience. This lack of elasticity allows for easier injury and the development of skin conditions, emphasizing the need for targeted treatment options to boost both collagen and elastin levels in older adults.
Impact of Environmental Factors
Environmental elements exert considerable influence on skin health. Chronic exposure to ultraviolet (UV) radiation, pollution, and other external irritants can significantly exacerbate senile dermatitis. UV rays cause direct skin damage, increasing photoaging effects, which manifest as redness and irritation.
Additionally, climate can impact the severity of dermatitis. For instance, dry or cold weather can lead to an increase in skin dryness, making the skin more vulnerable to dermatitis flare-ups. Hence, understanding these external factors allows healthcare providers to recommend effective protective measures, such as proper moisturizing techniques and sun protection strategies.
"The pathophysiology of senile dermatitis is not only a concern for dermatologists, but it also has broader implications for geriatric care. By elucidating the mechanisms of skin deterioration, providers can devise holistic treatment strategies."
In summary, the pathophysiology of senile dermatitis encompasses structural changes and the degradation of key skin proteins like collagen and elastin. Furthermore, environmental factors compound these effects, leading to an increased incidence of dermatitis in the elderly. An understanding of these dynamics is fundamental for developing effective treatments and prevention strategies.
Clinical Manifestations
Understanding the clinical manifestations of senile dermatitis is crucial for both diagnostic accuracy and effective management strategies. These manifestations provide insights into the underlying changes occurring in the skin due to aging, which can significantly affect the quality of life for elderly patients. Recognizing these symptoms enables healthcare professionals to tailor their approach and develop appropriate interventions. The evaluation of clinical manifestations also aids in distinguishing senile dermatitis from other dermatological conditions that may present similarly, ensuring that patients receive accurate diagnoses and effective treatments.
Common Symptoms of Senile Dermatitis
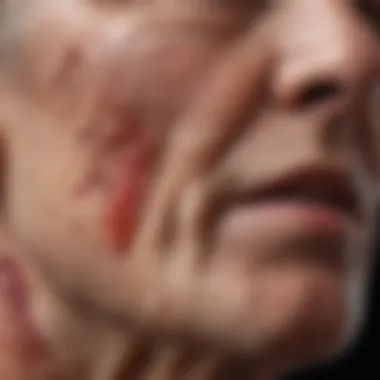
The symptoms of senile dermatitis can vary widely among individuals, but several common features consistently emerge across different cases. Typical symptoms include:
- Dryness and Flakiness: The skin tends to lose moisture, which can lead to a rough texture and visible scaling.
- Thinning Skin: As collagen and elastin fibers degrade, skin becomes thinner and more fragile, making it susceptible to tearing.
- Hyperpigmentation: Age spots, or liver spots, often appear on sun-exposed areas, reflecting increased melanin production.
- Redness and Inflammation: Irritation may occur, especially if the skin experiences friction or is exposed to irritants.
- Itching (Pruritus): Many patients report persistent itching, which can lead to scratching and further exacerbate skin damage.
These symptoms not only pose physical discomfort but can also lead to emotional distress for patients. Identifying these symptoms early is essential for initiating proper care and minimizing complications.
Differential Diagnosis
It is important to differentiate senile dermatitis from other conditions that can mimic its symptoms, such as eczema or psoriasis. Taking a thorough clinical history and performing a careful examination are critical steps in ensuring an accurate diagnosis. Key considerations in differential diagnosis include:
- Patient History: A detailed patient history can reveal previous skin conditions, family predispositions, and any medications that may contribute to skin changes.
- Appearance of Lesions: The specific characteristics, such as the location, color, and texture of skin lesions, help to distinguish senile dermatitis from other dermatoses.
- Response to Treatments: Assessing how the skin responds to various treatment modalities can further clarify the diagnosis.
"Accurate differentiation of senile dermatitis from other potential skin disorders is essential to provide targeted and effective management strategies."
The ability to recognize these nuances not only fosters better patient outcomes but also reinforces the need for continuous education within the dermatological community on aging skin conditions.
Ultimately, grasping the clinical manifestations of senile dermatitis lays the groundwork for developing a comprehensive management plan that addresses both physical and psychosocial aspects of patient care.
Diagnosis of Senile Dermatitis
Diagnosing senile dermatitis is critical for understanding the condition's nature and providing effective treatment. The aging population experiences unique skin changes that can lead to these dermatological issues. Recognizing the symptoms accurately is essential to prevent misdiagnosis or inappropriate treatment. This section discusses vital elements in the clinical examination and the role of biopsy in diagnosing this skin condition.
Clinical Examination Approaches
The clinical examination is often the first step in diagnosing senile dermatitis. A dermatologist will evaluate the patient's skin for various symptoms, including redness, dryness, and scaling. The approach typically involves:
- Patient History: Gathering information about the patient's medical history and any prior skin conditions.
- Visual Inspection: Observing the skin for characteristic signs of senile dermatitis. This may include examining areas commonly affected, such as the face, hands, and forearms.
- Assessment of Symptoms: Understanding the patient's experience regarding itching, pain, or discomfort.
- Physical Examination: Performing a thorough dermatological examination to explore the skin's texture, moisture levels, and pigmentation.
During the clinical examination, practitioners must distinguish senile dermatitis from other conditions, such as eczema or psoriasis. A thorough assessment can pinpoint specific characteristics that align with senile dermatitis, thereby ensuring that the appropriate treatment plan is established.
Role of Biopsy in Diagnosis
Biopsy can play a significant role in the diagnosis of senile dermatitis. When the clinical examination does not yield a definitive diagnosis, or when the symptoms are atypical, a biopsy may be necessary. This involves the following steps:
- Tissue Sampling: A small piece of skin is taken from the affected area.
- Histological Analysis: The sample is examined under a microscope to identify cellular changes that indicate senile dermatitis or rule out other conditions.
Biopsy provides crucial insights into the skin's structure and the presence of specific markers associated with aging. This method is particularly useful for determining the distinction between senile dermatitis and malignant skin conditions, which can mimic its symptoms. Ultimately, a biopsy can help dermatologists formulate a more tailored management strategy based on accurate diagnosis.
Understanding the diagnosis process is essential for effective intervention in senile dermatitis. By combining clinical examination with biopsy, professionals can enhance treatment outcomes for affected individuals.

Management Strategies
Managing senile dermatitis requires a comprehensive approach that takes into account the unique needs of the aging skin. As individuals age, their skin undergoes numerous changes that enhance the risk of various skin conditions. Therefore, employing effective management strategies is vital in preserving skin health and enhancing the quality of life for these individuals.
The importance of management strategies cannot be understated. They encompass a range of interventions that aim not only to alleviate symptoms but also to address the underlying causes of senile dermatitis. This holistic approach allows practitioners to tailor treatments to individual patients, providing a more personalized level of care. Moreover, effective management can significantly prevent complications, which are often more severe in older populations.
Topical Treatments and Their Efficacy
Topical treatments form the cornerstone of managing senile dermatitis. These treatments include moisturizers, steroid creams, and specific emollients. One of the primary goals of topical therapy is to restore the skin’s moisture barrier, which tends to deteriorate with age.
- Moisturizers: Essential for combating the dryness associated with senile dermatitis, they help to retain water within the skin. Products containing hyaluronic acid can be particularly beneficial due to their hydrating properties.
- Steroids: Mild topical steroids can reduce inflammation and soothe itchiness. However, long-term use should be approached with caution, as they may lead to skin thinning, especially in older adults.
Research shows that timely intervention with topical therapies can enhance skin appearance and reduce discomfort. Studies indicate significant improvements in skin hydration levels after consistent use of these products.
Systemic Therapies Considerations
In more severe cases of senile dermatitis, systemic therapies may be necessary. These are medications administered orally or injected, and they may include corticosteroids or immune-modulating agents. Systemic therapies can be effective for patients who do not respond adequately to topical treatments.
Before prescribing systemic therapies, healthcare providers should consider factors such as:
- Patient's overall health: The presence of comorbidities can affect treatment suitability.
- Potential side effects: Older adults may be more sensitive to side effects, so careful monitoring is essential.
- Drug interactions: Given that seniors often take multiple medications, it’s important to assess potential interactions carefully.
Utilizing systemic therapies can enhance patient outcomes when topical treatments fall short, but they require careful consideration and monitoring.
Lifestyle Modifications
Lifestyle modifications play a crucial role in managing senile dermatitis. Patients often respond well when they partake in habits that promote skin health. Simple yet effective interventions include:
- Hydration: Maintaining adequate fluid intake is essential for skin health. Encouraging patients to drink sufficient water daily can help keep the skin hydrated from within.
- Diet: Incorporating foods rich in antioxidants and omega-3 fatty acids can boost skin health. Foods such as fish, nuts, and fruits contribute positively to skin integrity.
- Sun Protection: Educating elderly patients about sun protection strategies is crucial. Daily use of sunscreen, wearing hats, and protective clothing can prevent further skin damage.
A proactive approach to lifestyle choices can enhance the efficacy of both topical and systemic therapies, promoting overall skin health among aging adults.
By integrating these management strategies, healthcare providers can significantly improve the well-being of patients affected by senile dermatitis. It is essential to remain vigilant and adapt treatments to address the evolving needs of elderly patients.
Psychosocial Impacts
Senile dermatitis affects not only the physical state of an elderly individual’s skin but also has significant psychosocial implications. These impacts can deeply influence a person's quality of life by affecting their emotional well-being and social interactions. Understanding the psychosocial dimensions of senile dermatitis is essential for comprehensive dermatological care. This section will elaborate on two critical aspects: the emotional effects on patients and the social stigmas they may face.
Emotional Effects on Patients
The emotional toll of senile dermatitis is often profound. Patients may experience feelings of frustration, sadness, and anxiety related to the visible signs of skin aging. These reactions are not merely superficial; they can lead to more severe mental health issues like depression. Patients may feel self-conscious about their appearance, potentially leading to a negative self-image.
Reports indicate that individuals with skin conditions, including senile dermatitis, are more likely to avoid social situations. This withdrawal can exacerbate feelings of loneliness and despair. Managing emotional health is crucial. Counseling and supportive therapies can be beneficial for those struggling with their self-esteem and overall mental health.
"Managing the emotional aspects of dermatological conditions is as important as treating the physical symptoms."
Social Stigmas and Isolation
The potential for social stigma related to senile dermatitis is another area of concern. Aging can already create feelings of marginalization, and when combined with visible skin issues, individuals may feel further isolated. The perception of society towards older adults with skin conditions often leads to misunderstandings and premature judgments.
This stigma can hinder personal relationships and professional opportunities. For elderly individuals, the fear of being ostracized or treated differently can result in social withdrawal.
Key factors contributing to stigma include:
- Perceived unattractiveness due to skin lesions or discoloration.
- Misinterpretations of skin conditions as poor hygiene or neglected health.
- Societal pressure to maintain a youthful appearance.
Addressing these stigmas requires educational efforts to enhance public understanding of senile dermatitis and its causes. Encouraging open conversations about skin health can help diminish stereotypes and foster a more inclusive environment for affected individuals.
Preventive Measures


Preventive measures in managing senile dermatitis are essential for maintaining skin health in an aging population. The skin undergoes various structural and functional changes with age, leading to increased vulnerability to damage. Implementing strategies to protect and care for the skin can mitigate these effects significantly. By focusing on prevention, healthcare professionals and individuals can improve the quality of life for older adults and reduce the occurrence of skin disorders.
Importance of Sun Protection
Sun protection is vital for preventing senile dermatitis. Prolonged exposure to ultraviolet (UV) radiation can accelerate skin aging and increase the risk of various skin conditions. Older adults often have thinner skin and decreased ability to repair damage, making sun protection even more crucial.
Key benefits of sun protection include:
- Reduces the risk of skin cancer: UV exposure can lead to skin cancer, especially for older adults, who may have accumulated years of sun damage.
- Minimizes premature skin aging: Regular use of sunscreen helps limit the formation of wrinkles, sun spots, and other signs of aging.
- Prevents skin inflammation: Protecting the skin from UV rays can help reduce flare-ups of conditions such as senile dermatitis.
To effectively protect the skin, older adults should use broad-spectrum sunscreen with a high SPF. This should be applied generously and reapplied every two hours, or more frequently if sweating or swimming. Wearing protective clothing, wide-brimmed hats, and seeking shade during peak sun hours are additional strategies that can enhance sun protection.
Hydration and Skin Care Routines
Proper hydration and a consistent skin care routine are fundamental in preventing senile dermatitis. Aging skin tends to lose moisture more rapidly, leading to dryness, irritation, and increased susceptibility to dermatitis.
Effective hydration strategies include:
- Using moisturizing products: Emollients can help replenish moisture and create a protective barrier. Look for creams or lotions that contain ingredients like hyaluronic acid or glycerin.
- Maintaining adequate water intake: Staying hydrated from the inside can significantly impact skin health. Drinking enough water is essential to support overall bodily functions and skin elasticity.
Additionally, a simple and effective skin care routine can help in maintaining skin health:
- Gentle cleansing: Use mild, fragrance-free cleansers to avoid irritation. Harsh soaps can strip the skin of natural oils, worsening dryness.
- Regular moisturizing: Apply moisturizer immediately after bathing to lock in moisture.
"Preventive care can be less costly and more effective than treating conditions after they develop."
Overall, integrating sun protection and a comprehensive skin care routine into daily life can significantly impact the health of aging skin. Emphasizing these preventive measures will not only improve the appearance of the skin but also enhance the overall well-being of older adults.
Future Research Directions
Understanding senile dermatitis is a multifaceted endeavor that requires ongoing research. The topic of future research directions is vital for clinicians and researchers alike, as it paves the way for innovations in diagnostics, treatment, and prevention. By identifying the areas that need further investigation, we can improve care for older adults affected by this condition. The implications of potential research extend beyond mere knowledge enhancement; they include applications that can transform clinical practices.
Emerging Therapies and Innovations
The landscape of dermatological treatment is continuously evolving. New methodologies and therapies are on the horizon, focusing specifically on senile dermatitis. For example, biologic therapies targeting inflammatory pathways show promise in managing skin conditions linked to aging. Researchers are also investigating the use of stem cell treatments to regenerate damaged skin. Emerging technologies like teledermatology are making consultations more accessible, especially for aging populations with mobility issues.
- Advances in topical formulations can provide more effective relief for symptoms associated with senile dermatitis.
- Innovations in patient education tools aim to enhance individual understanding of skin care routines that best suit aging skin.
"Investing in research is investing in the future of skin health for elderly populations."
Simple studies on genetic predisposition can also unveil why some individuals are more susceptible to senile dermatitis. Insights gleaned from this research can help in tailoring preventive measures to individual needs.
Gaps in Current Knowledge
Despite the progress made, significant gaps still exist in our understanding of senile dermatitis. One key area needing attention is the lack of standardized diagnostic criteria. Current diagnoses often depend on subjective clinician interpretation rather than objective measures. This inconsistency creates challenges in comparing treatment outcomes across studies and clinical settings.
Another major gap is the under-representation of diverse populations in clinical trials. Most research has focused primarily on Caucasian subjects, limiting the applicability of findings to other ethnic groups. Additional research is necessary to understand variations in both prevalence and treatment response among different demographics.
Furthermore, the psychological impact of senile dermatitis should be examined more rigorously. Many older adults experience emotional distress associated with visible skin changes, yet few studies address this aspect comprehensively. Bridging these gaps can inform holistic care approaches that consider both physical and emotional aspects of aging skin health.
Culmination
In the journey to understand senile dermatitis, it becomes clear that this condition is not merely an aesthetic matter but a significant health concern among the aging population. The complexities surrounding senile dermatitis lie in its multifactorial origins, manifesting from intrinsic aging processes and external environmental influences. Recognizing the importance of this condition aids not just in enhancing the quality of life for the elderly but also in tailoring precise dermatological care that accommodates their unique needs.
Summary of Key Points
The exploration of senile dermatitis reveals several crucial points:
- Definition and Importance: Senile dermatitis is a collective term for skin changes associated with aging, underscoring the necessity for awareness in both medical and social spheres.
- Epidemiology: The condition affects a large segment of the elderly population, necessitating targeted research and treatment strategies tailored to different demographic groups.
- Pathophysiology: Understanding how skin structure changes with age, specifically in relation to collagen and elastin, is essential in grasping how these alterations lead to various symptoms and clinical manifestations associated with senile dermatitis.
- Management Strategies: An effective approach should include both topical and systemic therapies, along with lifestyle modifications, to optimize outcomes and improve skin health in older adults.
- Psychosocial Factors: The emotional and social impacts of senile dermatitis must be acknowledged, as they play a significant role in the overall well-being of patients.
- Preventive Measures: Simple preventative strategies, such as sun protection and proper hydration, can significantly improve skin health and quality of life.
Call to Action for Future Studies
The exploration of senile dermatitis must not remain static; future research directions should focus on several key areas:
- Innovative Therapies: There is a pressing need for the development of new, more effective treatments targeting the pathophysiological mechanisms underlying senile dermatitis. Investigating emerging therapies could yield beneficial results.
- Gaps in Knowledge: Current literature presents many gaps that require further elucidation, particularly regarding the psychosocial dimensions of senile dermatitis and its implications for quality of life among the elderly.
- Collaborative Research: Encouraging collaborations between dermatologists, gerontologists, and researchers is vital to deepen the understanding of senile dermatitis and enhance its management.
Expanding our knowledge base through dedicated research can create an impact that resonates beyond academics. It can lead to clinical advancements that not only enhance healthcare practices but ultimately improve the lives of those affected by senile dermatitis.







